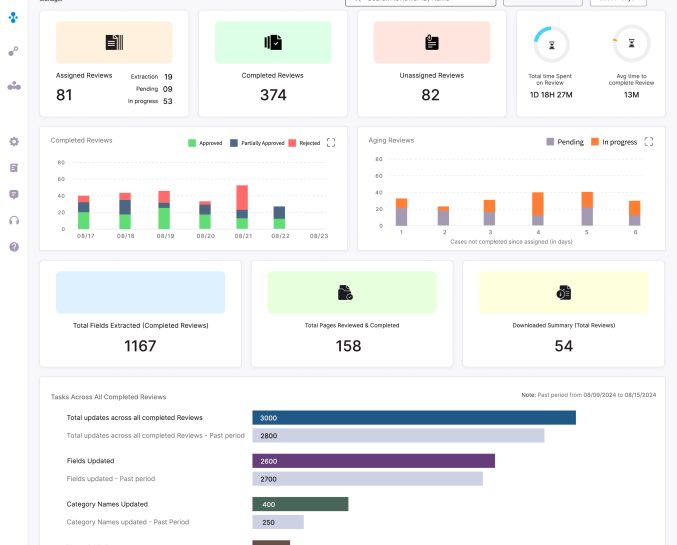
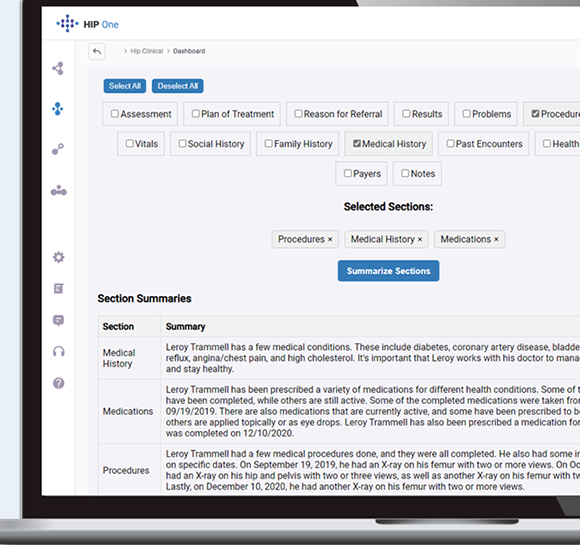
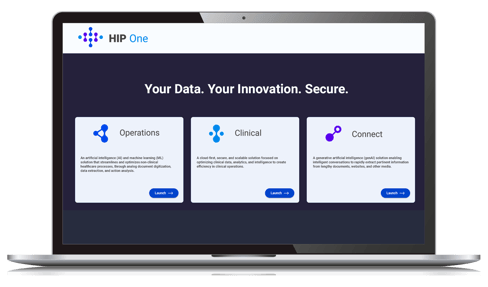
Genzeon goes beyond basic automation by embedding clinical reasoning and intelligent decision-making directly into claims and medical review workflows. Instead of only digitizing documents, HIP One interprets data, recommends actions, and accelerates resolutions.
HIP One also integrates seamlessly with existing systems and adheres to industry compliance and security standards, ensuring a smooth transition and reliable performance across your enterprise workflows.